
Definition
Athlete’s Foot: A fungal infection of the foot's skin, especially between the toes.
General Info
Athlete’s foot, also known as tinea pedis, is a fungal infection of the feet. In most cases, the fungal infection develops on the bottom of the foot and between the toes. Athlete’s foot is a common health problem that may last for a long time if the proper care and attention is not applied. This condition can be difficult to treat and may recur following treatment.
It's commonly believed that athlete’s foot is contagious and that a person can pick up the tinea fungus by touching an infected individual or by walking on damp floors in areas with heavy foot traffic, such as locker rooms or public showers. In truth, though, fungi live on many surfaces, including the skin. What makes a person become infected is reduced immunity (there are many possible causes of this) in combination with a foot environment in which fungi thrive (i.e., a warm, dark, and moist environment).
In some cases, athlete’s foot may be caused by a bacteria instead of a fungus. Bacteria-related athlete’s foot may require antibiotics instead of anti-fungal medication. Certain health problems—psoriasis, dermatitis—may look like athlete’s foot but do not improve following the use of anti-fungal medication.
Signs & Symptoms
Frequently experienced signs and symptoms associated with athlete’s foot include:
- Foot odor
- Foot rash
- Bumps on the feet
- Itching, burning, or pain in the affected areas
- Redness and scaling on the bottoms of the feet
- Cracks, blisters, or peeling areas, usually between the toes
Possible Causes
Some of the most common causes of (or factors that contribute to) athlete’s foot include:
- Reduced immunity
- Excessive sweating
- Minor skin or nail wounds
- Allowing the feet to remain wet for prolonged periods
- Wearing closed-toe shoes, especially if the shoes are plastic-lined
Athlete’s foot is common in people who wear constrictive shoes or boots. This type of closed-toe footwear causes the feet to sweat and creates a warm, damp environment in which fungi can grow. Athletes are particularly susceptible to athlete’s foot, due to the accumulation of sweat on their feet and in their shoes while practicing or competing.
It is now widely accepted that fungal skin infections can lead to fungal infections of the toenails—a condition called onychomycosis. Onychomycosis causes the toenails to become thick, discolored, inwardly curved, and painful. Diabetics should be particularly concerned with athlete’s foot, as the fungi-related skin damage associated with this health problem can allow bacteria to invade the skin and cause a life-threatening infection or the need for an amputation.
Helpful Strategies
Conventional treatments for athlete’s foot involve the use of certain oral and topical medicines. While oral anti-fungal medications are commonly prescribed for this condition, they are hard on the liver, and it may be better to try topical treatments first. If oral medications are used, it’s important to regularly monitor liver function with lab tests. Note: Individuals who use topical anti-fungal medications should apply it just before bedtime and cover it with saran wrap to aid penetration of the substance into the infected skin. Also, many over-the-counter anti-fungal sprays or creams may not help eliminate athlete’s foot, as they do not attack the correct fungus or are simply not strong enough to eliminate the foot fungus.
One of the most important factors in treating and preventing athlete’s foot is creating a foot environment that is light and dry, not warm, dark, and damp. Consider wearing sandals in place of closed-toe shoes as much as possible to create a foot environment in which fungi cannot thrive. Wearing sandals exposes foot fungus to the sun's lethal ultraviolet rays.
Keeping the feet dry may also be an effective strategy in treating or preventing athlete’s foot. Keep some dry socks handy and change socks regularly to help mitigate fungal growth. Socks made of newer synthetic materials may help wick moisture away from the skin, which helps inhibit fungal invasion. Individuals whose jobs or hobbies require the use of constrictive shoes or boots should consider buying a shoe dryer.
Since skin has inherent immune properties, skin itself helps ensure that exposure to fungus does not lead to infection. So, to this end, it’s important to make sure that immunity is optimized. Talk to a natural healthcare provider about ways to improve immune system health.

WANT TO IMPROVE YOUR FOOT HEALTH?
Let the team at Natural Footgear help you! Subscribe to our newsletter for the latest offers and helpful info, and sign up for our FREE email courses on various topics and foot health conditions.
Sign Up →
Want to Improve Your Foot Health?
We are here to help you every step of the way. Get our newsletter for the latest offers and helpful info, and sign up for our FREE email courses on various topics and conditions, including bunions, hammertoes, neuromas, plantar fasciosis, shin splints, ingrown toenails, and more.
Sign Up →
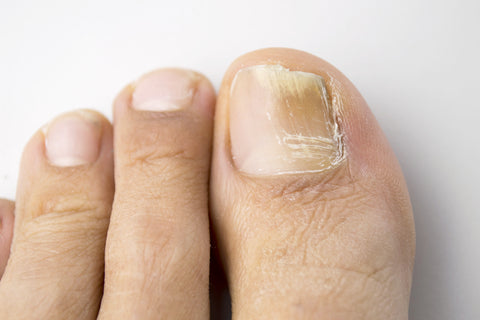 Several factors may cause or contribute to foot and toenail fungus, including conventional footwear, decreased immune function and circulation, and trauma. Fungal toenail infections, also called onychomycosis, are common in adults and typically follow fungal infections of the feet. Fungal foot and nail infections can be difficult to treat and may recur even after successful treatment. Here are some additional details about the three factors mentioned above that may cause...
Read more
Several factors may cause or contribute to foot and toenail fungus, including conventional footwear, decreased immune function and circulation, and trauma. Fungal toenail infections, also called onychomycosis, are common in adults and typically follow fungal infections of the feet. Fungal foot and nail infections can be difficult to treat and may recur even after successful treatment. Here are some additional details about the three factors mentioned above that may cause...
Read more











Hello! I loved reading this article. It gave me some good tips for if I develop athlete’s foot. I had it once as a kid, but ever since then, I’ve avoided it. If you develop it in a warm climate or during a warm part of the year, the best thing you can do is wear sandals as opposed to enclosed shoes, especially with socks. A light, open shoe will definitely allow the feet to breathe and help them get back in shape, and I think sandals are especially comfortable anyway, particularly when you’re outdoors and a light breeze blows on the feet. Even if you’re not a sandal-wearer, give them a try if you have athlete’s foot. You won’t be disappointed and you may want to stick to wearing them!
Thank you for your comment, Dan! It’s hard to beat the combination of a dry environment for the foot and exposure to sunlight in addressing athlete’s foot. Foot-healthy sandals are an excellent option for the scenarios you mentioned!
All the best,
Robyn Hughes, ND
I’ve been fighting athlete’s foot on and off again for years. I’m especially having a hard time finding slippers to wear around the house and after taking showers. Aren’t there any slippers out there that can be recommended? Like, something made out of bamboo or some other magical fungus-resistant material? Any suggestions, Dr. Hughes?
Hi, Ellen,
Thank you for your comment. One brand of slippers that we use and like is called Glerups. These slippers are made of wool, which is advantageous for a number of reasons, including wool’s ability to absorb moisture and keep your feet dry. Of course, an open-toe option, such as a flip-flop, could also work, provided the slipper or sandal is sufficiently secure on your foot. This would allow more light to reach the affected area(s) and assist in managing the problem.
Kind regards,
Robyn Hughes, ND